HOSPITALITIS
 None of us can ever forget our initial trip to the hospital for myocarditis. I think fear was the most pressing emotion for all involved: family and patient alike. Staff tried to allay our fear with reassuring words, but they fell on deaf ears. Deep down, I knew whatever this was, it was a game-changer. The question was, would I be able to face it. I remember thinking that I just didn’t think I would die so soon. My overriding concern was not for myself but for my family, leaving them behind. I had no idea what the disease was or how much history, innovation, and bravery had contributed to my survival.
None of us can ever forget our initial trip to the hospital for myocarditis. I think fear was the most pressing emotion for all involved: family and patient alike. Staff tried to allay our fear with reassuring words, but they fell on deaf ears. Deep down, I knew whatever this was, it was a game-changer. The question was, would I be able to face it. I remember thinking that I just didn’t think I would die so soon. My overriding concern was not for myself but for my family, leaving them behind. I had no idea what the disease was or how much history, innovation, and bravery had contributed to my survival.
All the medical stuff that subsequently happened was a difficult journey, made bearable by the compassion of the staff who choose to take care of the most complex patients. Across the board, every level of staff, every diverse function of staff, all were wonderful to me. I embraced their kindness. I gulped it into my lungs like oxygen, fueling my ability to cope. Lots of routine visits, tests, medications, crises averted, and more than twenty years later, I end up with many hospitalizations over the recent 2-3 years, thanks to COViD and lots of circulating viruses, which have disproportionately affected those of us who are immunocompromised.
Have things changed in medicine over these past two decades? Yes of course. The use of Nurse Practitioners and Physician Assistants has taken a lot of pressure off both doctors and nurses and contributed greatly to the comfort of the hospitalized patient. All that I have met, have been extremely knowledgeable and professional, not to mention, they are available off shift, throughout the night to address issues as they arise. The Myocarditis Foundation, under the leadership of Executive Director Gen Rumore, has made a concerted effort to educate Nurse Practitioners about myocarditis as their observation and insight is often the first member of the medical team to recognize untoward and unusual cardiac symptoms and bring them to the doctors’ attention. This program is an extension of the Foundation’s mission which is to educate medical professionals about the disease.
I’ve managed to be hospitalized twice over the Christmas/New Year’s holiday. When there was not a single car parked on Fort Washington Avenue outside my window, yet there was always adequate staff in-house to care for me, for everyone. One Christmas Day I had the television on the channel that pictured a fire burning in a fireplace while playing Christmas Carols, watching to snow fall outside my window. It was the best I could do to celebrate my favorite holiday.
The COVID pandemic continues to create problems for hospitals, necessitating procedural flexibility, like housing two patients in an Isolation Room intended for one. All changes in protocol were necessary to care for the overwhelming caseload of infected, seriously ill patients. It will take years of retrospective studies to fully understand this crazy pandemic and how it affected the world. The fall out will likely include the closure of many hospitals, I fear mostly in economically disadvantaged neighborhoods, after caring for the uninsured. Many have opined that our medical system was broken, even before this happened. Equity in medical care of all economic strata should be our goal.
With each respiratory virus, I was discharged as soon as I started to improve, sent home to convalesce to prevent me from acquiring a different, hospital-based infection. Also, the bed was desperately needed for the patients in the ER who had been waiting for days for a bed upstairs. I remember being conflicted regarding whether I felt well enough to manage my disease at home versus staying in their very excellent care but at risk to picking up something new and quite possibly worse. The decision was mine; but of course, I always chose going home to be with family with the proviso that I could return at any time if I deteriorated.
My prediction is that hospital care and medical care, will continue to change in coming years as money becomes more scarce and hospital administrators try desperately to deliver a high standard of care with fewer resources as insurance companies and the government try to limit options by controlling spending through withholding treatment approvals. Myocarditis patients in profound heart failure require what I’ve always described as the use of “every tool in the toolbox” in order to survive. I pray that these cutbacks in hospital services will not affect the innovation, discovery and delivery of medicines, devices, services, and staff who are needed to care for very sick myocarditis patients. We transplant patients live because of the “The Hard and Glorious Journey” (as stated in the “Heart Transplant” research article by Dr. Stolf, published in 2017) undertaken sequentially by creative and skilled physicians over more than 50 years, each building on each other’s discoveries, bringing us to where we are today, leading to longer survival. Meanwhile, the Myocarditis Foundation will continue to fund research utilizing your donations, to guarantee that innovation with the goal of finding a cure, will continue.
SEASONS OF DISCONTENT / LIFE OF JOY
 Looking back on almost 23 years of transplant life, I can almost put the issues I’ve faced into three sequential buckets.
Looking back on almost 23 years of transplant life, I can almost put the issues I’ve faced into three sequential buckets.
The first seven years were rejections: 5 severe and roughly 10 of lesser grade. Lest you think I was incapacitated in-between those episodes, I wasn’t. They were some of my best tennis years. They were also the years of my son’s wedding and the birth of my first grandchild. Tumultuous yes, however, in perspective, incredibly wonderful. Exactly what I had prayed to live to see.
The next seven years could be placed in the bucket of palpitations/arrhythmias/AICD changes. Never did they exactly figure it out, but one day these unpleasant episodes just stopped. And during these times, there were lots of medication changes and subsequent side effect management. My bloodwork is never completely normal, but I have more than 20 years of data to prove that I am normally abnormal. Again, on the home front, these years were also amazingly wonderful; another wedding, more grandchildren, singing in church choir, travel, physical fitness – happy to be alive.
These last 7 years could be characterized medically as more complicated which has mirrored my personal life. Frequent hospitalizations with great diversity of infectious agents, the passing of significant and beloved family, cancer treatment of family and friends very close to me, as well as celebrations of 50 years of marriage and crossing the line to old(er) age. It never occurred to me that I would experience life as an older person; I never dared dream that I would be referred to as “Mam” (madam), stand crooked, walk with a cane, go to bed early, eat dinner at 5 pm, but I do, and I feel blessed to do so. I benefitted from the advances in our understanding myocarditis and transplant medicine over that time. Time to think of my legacy.
Through it all, it has been my honor to serve the Myocarditis Foundation in many capacities, to meet so many wonderful people like you, to become acquainted with talented and caring physicians from all over the world who are also committed to serving patients and families like you and me. I am grateful for the service to our foundation of folks like Gen and Joe Rumore, who currently run the day-to-day operations of the foundation as Executive Director and Chief Operating Officer respectively. It is the same for us all, the Board, Dr. Cooper, Dr. Price and the Medical Advisory Board, members past and present, that serving the foundation is much more than a job or a volunteer effort. It is a calling; one we didn’t pick, but that picked us. We share this legacy.
Someday there won’t be any need for a foundation like ours, the day we collectively find a cure. What a glorious day that will be. The MF has been the driving force in progress in understanding this disease and we will not leave our post until we are no longer needed. Consider making a recurring donation, hosting a fundraiser or leaving a legacy gift. We cannot do this without your help.
Trust that we are working, have been working and will continue to work on the disease that disrupted, detoured, complicated and in the cases of some families, tragically destroyed their lives.
In the meantime, let me leave you with this story about giving that I found in multiple sources on the internet, slightly revised:
“Once upon a time there were four people: Everybody, Somebody, Nobody and Anybody. There was an important job to be done. Everybody was sure Somebody would do it. Anybody could have done it, but Nobody did it. Somebody got frustrated about that because it was Everybody’s job. Everybody thought Anybody could do it, but Nobody realized that Everybody did not do it. It ended up that Everybody was sure Somebody would when Nobody did what Anybody could have, and Everybody should have.”
Fundraising for myocarditis, a previously unknown disease, has been a challenge through the years. We are grateful for Everybody who has given over the years. The foundation just received a Platinum Transparency Certification from Candid, formerly Guidestar, so you can be assured of our effective management of donations. Fundraising events throughout the pandemic all but ceased. Grant money also remains challenging as corporations narrow their giving to specific geographic areas or populations. Everybody thinks Somebody else is giving. We need you to be the Anybody who did! Giving feels good. Join us and choose to make eradication of this disease your legacy too. It will bring you great joy.
New Year’s Resolutions You Can Keep
 I never met a New Year’s Resolution I could keep. And it’s not like I could forget it as it was always the same: Lose weight and exercise more. That is until I found this article online and have adapted it to heart transplant patients like us. The dictionary defines “resolution” as a firm decision to do or not to do something. Reflecting on the past year, makes us want to do the New Year better. However, life is full of twists and turns. See if you find any of this helpful.
I never met a New Year’s Resolution I could keep. And it’s not like I could forget it as it was always the same: Lose weight and exercise more. That is until I found this article online and have adapted it to heart transplant patients like us. The dictionary defines “resolution” as a firm decision to do or not to do something. Reflecting on the past year, makes us want to do the New Year better. However, life is full of twists and turns. See if you find any of this helpful.
1. Commit to staying in relationships with your tribe, be that your family, or close friends, or folks you know from your house of worship. A famous Gallop poll done in 2020 revealed that American citizens reported their own mental health at an all time low. I think we are at even greater risk for our mental health to be compromised due perhaps to PTSD caused by a sudden detour in our lives from myocarditis, from side-effects of our meds, from fear of an uncertain future, from frequent illnesses or uncertain finances from the cost of our care. Don’t isolate when it’s medically allowable for you to be in community; stay in touch; let yourself receive support when offered, and freely give it away.
2. As much as possible, grow comfortable with being flexible. I optimistically pay for tickets for plays, concerts, trips, entertainment every year, and end up giving them away when I get sick. Little things used to throw me: a long wait for a test, my required meds not coming in the time I was expecting, or serious traffic on my way to a clinic appointment. As transplants, we must be committed to taking meds on time, scheduling and keeping appointments, making sure we eat right and exercise daily. But stuff happens; some things you just can’t control. Forgive the universe for the intrusion and move on. Don’t make yourself a victim.
3. Slow down; take time to rest, refuel; give yourself a break. Treat yourself; sleep in. We’re so overscheduled in our society today that we don’t have time to even think. Spend time caring for you, doing what you love. I love to bake for shut-ins or make a meal for someone who is in need. When my grandchildren are coming, I like their first awareness when entering my home, is to smell a special dessert baking in the oven. It makes me excited and calm at the same time. Take your dog for a walk; he’ll love it.
4. Speak in hope. If you find yourself being negative, turn off the TV. Count your blessings. Encourage others. Volunteer for an organ donor organization. Do more listening than talking. Live with gratitude. Count your blessings. If you can’t graduate to a more positive mindset, talk to your doctor about medication or perhaps counseling. It always good to learn more about how you tick. Meditate. Pray for others less fortunate than you.
5. Love your neighbors. Be kind. Reach out to others you know are hurting. I believe that there is always someone out there who is worse off than I am. Nothing makes me feel better than to do something for someone else. Clean your closets, donate items to an organization that helps the poor.
Well, what do you think? I’d love to compare notes with you at year end. These are a few resolutions I can really get behind. Believe me, you are worth it!
Vaccines
In my ongoing quest to learn new information about my disease, Giant Cell Myocarditis, so that I can be helpful to others who have followed me, Dr. Cooper put me in touch with a physician with expertise in immunology. The Center for Advanced Cardiac Care would like me to have two fairly new immunizations for diseases which could take me down if I contracted them. You may remember that I originally succumbed to GCM within two hours of being immunized with Typhoid and Hepatitis A, which were required for me to travel to Malawi to do mission work 22 years ago. For about ten years following the transplant, I didn’t receive any immunizations at all until SARS (the precursor to COVID) showed up, carrying an existential threat to people like me.
Thus began my lifetime pursuit of researching all immunizations being recommended by my physicians, reflexively given in Emergency Rooms for even minor injuries, or advertised on TV for people my age for the presence of an aluminum adjuvant. I read package inserts, consult pharmacists, have contacted pharmaceutical companies for product information, gathering intelligence to help me make my decision whether or not to have the vaccines.
What would have happened if I’d only had one and came back for the second at a later date? Who knows. I got short of breath when doctors and pharmacies recommended getting the flu and Covid vaccines at the same time this year. You can come back for the second one. You are in the driver’s seat.
The statistics were on my side 22 years ago. “The vaccines you are receiving have been used for years, worldwide, have been administered to millions of people, and are very safe”, my doctor said in August 2001. Turned out not to be true for me.
I just got off the phone with a retired Colonel in the US Army Medical Corps, a medical consultant in a variety of disciplines. She is an allergist/immunologist/Vaccinologist-Adversomics with encyclopedic knowledge of myocarditis, vaccines, and adverse events related to them. We talked about lots of other things too: the state of healthcare in the United States, vaccine-acquired immunity versus vaccines preventing severe complications of the disease, adverse event reporting of vaccine injuries, and immunological health. Some of the facts are sobering: the #1 cause of bankruptcy in the U.S. is healthcare debt; the United States ranks 35thin infant mortality in the world; not all adverse events are listed in the package insert.
Vaccine injuries should be reported. If your physician doesn’t report them, you can. I get my vaccines at one of the large pharmacy chains. You must sign a consent first. Read it carefully. At the same time, you should receive an information sheet which explains how to make an injury claim. Vaccine Injury Reporting and Compensation is a federal program administered by the US Department of Health and Human Services. Before receiving a vaccine of any kind, please consult your post-transplant physician.
The expert I talked to opined the following: “Did you know that love, kindness and forgiveness help create immunological health?” I have long felt that a positive mind-set creates a healthy environment for a foreign heart to feel at home in your body. It was affirming to meet someone who thought the same way I do about health, though I never considered specifically immunological health.
Though immunized, I am currently fighting my way through the flu, trying to stay out of the hospital yet again. Now armed with new information about vaccines and learning that they can also play a role in preventing serious complications of the disease, I can hopefully slide toward an uncomplicated recovery at home.
In the New Year, I have a renewed gratefulness for doctors and researchers who devoted their lives to studying immunology, myocarditis, vaccines and other issues that affect our transplanted lives.
By Candace Moose, Co-Founder
Navigating the Emergency Room
For the 5th time in the past two years, I was admitted to the hospital with yet another esoteric respiratory virus that hampered my breathing. I have tons of medications that have been prescribed for me to manage my asthma symptoms at home, but when my PO2 drops to a certain level and my tidal volume falls beneath my doctor’s allowable range, I must go to the Emergency Room.
Going to the ER is always a traumatic experience for me. First, you never know how long you are going to be there. At my hospital, where the beds are almost always full, you could be there for several days. I always assume I’m going to be admitted, so I pack of suitcase with essential items: a mask, my phone charger, my bathrobe which can act as a blanket or a pillow, my meds, slippers, toiletries, bottles of water and some packaged snacks. In different parts of the ER there is no cell phone coverage, so during COVID, your family left you in the ER waiting room and then didn’t hear from you for sometimes days before you were transferred to a room upstairs somewhere. Meanwhile, no one is filling a pitcher of water at your bedside, but in my admission to the ER most recently, I found the ice machine which I could refill myself, so at least I was hydrated. First, I was placed in the hall, then put into a two-bedroom designed for one patient, with one call bell for the nurse and one TV control, which was already in the possession of the other patient. Oh, also when packing your suitcase, pack a whole lot of patience. As a nurse and immunosuppressed transplant patient, I was frightened of the variety and severity of obvious illnesses around me, but I tried not to let my mind wander to the “what ifs”. I keep reminding myself that I am in one of the most renowned hospitals in the most advanced country in the world. As grateful as I am, I think it could be done better.
However, let me reassure you that the ER is well staffed and everything that is ordered for your emergency care is delivered professionally and quickly. If you are still not okay, speak up, let somebody know. Your needs will be rapidly addressed.
Eventually, I was transferred to a private room upstairs because I was considered infectious. While writing this I realize now how insensitive I was not to realize I was the dangerous one to many of the other patients. Forgive me. When I arrived on the floor, I had been awake for ten days, coughing, taking medicine to help me breathe through the night. Laying down made me cough more. It was 6 am. I did what any other self-respecting patient would do, and offered the very sharp Nursing Assistant who got me set up in my new room, the deed to my house for a cup of coffee. She was thrilled and asked to see pictures of what she would soon own. I said, “Oh, by the way, it comes with a hypo-allergenic dog and a wonderful husband.” She definitely didn’t want the dog and wasn’t sure she wanted the husband either. I told her she may want to wait to decide until she met him because he’s really good looking. We laughed every time we crossed paths over the next five days.
I’ve been at this for 22 years. It’s never easy but when you can start laughing at the little stuff, it helps to cope with all the big stuff that is not going right. In this flu, COVID, RSV, and virus-ridden holiday season approaching, I wish you health and laughter!
PS: If you need me, I’m available to talk. Contact the Myocarditis Foundation office. I’m pulling for you.
Sending all my love,
Candace
Never Forget
 September is my birthday month. 22 years ago, on my birthday, I was in the Critical Coronary Care unit in northern Manhattan, catastrophically ill, receiving intravenous chemotherapy. The doctors were not sure I would live through the night. I remember every detail of that day, even so many years later. However, what was happening to me, was unimportant compared to what was happening downtown the following day.
September is my birthday month. 22 years ago, on my birthday, I was in the Critical Coronary Care unit in northern Manhattan, catastrophically ill, receiving intravenous chemotherapy. The doctors were not sure I would live through the night. I remember every detail of that day, even so many years later. However, what was happening to me, was unimportant compared to what was happening downtown the following day.
The staff let my husband spend the night in the chair next to my bed because it was my birthday. Jim turned on the television the next morning, and we watched the planes hit the World Trade Center towers. All of a sudden, the chest pain I felt was not cardiac in nature, but rather a physical manifestation of grief for the overwhelming loss of lives that happened that day. I prayed for the country and for our President. Every year since, the feelings are the same. In the midst of our personal tragedy, 2753 souls perished following a stunning act of terrorism. The day devolved from there, revealing multiple coordinated attacks.
As a patient lying in a bed in one of the most revered medical institutions in the country, not only did I not know whether or not I would live, I also didn’t know if our country was at war. All of the other patients in the CCU were moved out of the unit to make room for survivors, I suspect as part of the city-wide Disaster Plan.
The authorities closed all the tunnels, bridges, subways and roadways leading in and out of the city and all phone lines were cut. Jim was stranded sleeping on the floor of the Waiting Room for several days. My family didn’t know if I had lived or died. My nurses however came to work every day past the roadblocks, past the military check points, away from their families, to care for me. I could never forget their professionalism, their courage, and their faithfulness.
I will never forget.
Short Cuts

It’s a curious thing, being a transplant. I don’t know how to answer the often-asked health survey question, “What do you consider your current health status to be? “And the choices are excellent, very good, good, fair, or poor. If you’re asking me on a good day, I feel quite excellent. But am I? As a transplant, are you like everyone else, excellent in the absence of a crisis? When I go to an Emergency Room other than Columbia Medical Center, doctors are either scared to death of me or confidently casual. I’m afraid of both. They either over or under medicate, both have the potential to be life-threatening to me. I had a local ER instruct me not to come back, stating that their focus was not to treat a complex patient like me. I appreciated their honesty.
I’ve spent 50 years of my life being like everyone else, and 22 years being a “complex” patient. Things that normal people are casual about, I can’t even consider. I’m tossing around the idea that I may not travel by air anymore. Between crowded terminals and planes, I just don’t belong in such close quarters. I easily get really sick. Another example is drinking alcohol. I used to enjoy wine, or a margarita. Now alcohol makes me sick. I’m on so many toxic drugs that my system just can’t handle it.
So many healthy people want to bypass signs of aging; for example, using dermatology medications and procedures to make them look younger. Or medical or surgical interventions for weight loss. We do put on weight when we age. We’re less active; in my case my fear of falling interferes with my independence. But wrinkles, and weight gain, and many other issues are normal conditions of an aging body. My astute five-year-old grandson observed that I was more jigglie and wrinklie than his mother. Can’t argue with that.
Aging as a transplant is a really good thing; the alternative, not so much. Potential transplant recipients go through rigorous presurgical physical, mental, social, and financial screening to determine if they can handle the transplant life. It isn’t easy, even though we make it look that way. There is no half-way. There are no short cuts. You’re either in or out. When issues pop up at this age, I’m never really sure now whether they are a transplant issue or one that occurs in the normal course of aging.
I spoke to a transplant cardiologist friend of mine who predicted that at some time in the future they would no longer perform heart transplants because artificial hearts and other mechanical devices will be perfected. No immunosuppressive drugs. That is really something to look forward to.
The Myocarditis Foundation emphasizes that heart transplants are not a cure for myocarditis but rather a treatment, the only treatment available for the sickest patients. Their work must continue until a better solution becomes standard of care. Please support the ongoing cause.
For me, as long as I keep my eyes on heaven and my heart focused on helping others, with my family, friends, and my Advanced Cardiac Care Team by my side, I’ll be okay. My Grandfather, who I adored, used to say I was “solid”. I never asked him exactly what he meant; solid physically (which I am) or emotionally (which I am also). I’ve been tried and tested, sometimes beyond my ability to cope at the moment, but I’ve rebounded, recovered and persevered. I wish you strength.
Mind and Body Connection
 Years ago, when I was in CCU waiting for/hoping for an organ, in addition to all the heart failure drugs, I was placed on intravenous chemotherapy to treat the Giant Cell Myocarditis. Because I was afraid of it, I listened to a meditation tape via headphones, while it was being infused. I imagined the medication was coming into my body, and like Pac Man, was eating up the lymphocytes and Giant Cells that we not supposed to be there. I pictured stars and light being infused into my body to bring me health and healing. There was no other way for me to live as the medication was intended to try to keep me alive long enough to receive a transplant; a bridge to transplant, not a cure. Dr. Cooper’s prior research had revealed this truth. Sometimes we have to imagine and believe that the medicines that make us sick were prescribed to help us.
Years ago, when I was in CCU waiting for/hoping for an organ, in addition to all the heart failure drugs, I was placed on intravenous chemotherapy to treat the Giant Cell Myocarditis. Because I was afraid of it, I listened to a meditation tape via headphones, while it was being infused. I imagined the medication was coming into my body, and like Pac Man, was eating up the lymphocytes and Giant Cells that we not supposed to be there. I pictured stars and light being infused into my body to bring me health and healing. There was no other way for me to live as the medication was intended to try to keep me alive long enough to receive a transplant; a bridge to transplant, not a cure. Dr. Cooper’s prior research had revealed this truth. Sometimes we have to imagine and believe that the medicines that make us sick were prescribed to help us.
I believe that how we think about our medications, procedures, hospitalizations, and complications may affect the outcome. We stumble, we fall, we feel afraid, but we pull it together and get out heads on straight. Otherwise, the uncertainty, the constant threat to our existence, and the discomfort will overwhelm us and interfere with our ability to cope, and in consequence, interfere with our ability to experience the joy and gratitude for the extended life we have been given.
I make up stories about the pills I take daily. Some of them seem to sing. I have favorites, particular shapes or colors. I happen to love gummy vitamins because I get to eat candy without guilt. Conversely, the calcium supplements I don’t like. They’re chalky, large and dry, difficult to swallow. I usually figure out pretty quickly which new drugs I can’t tolerate. I got GCM because of an autoimmune reaction to vaccines, so over the years, I’ve had lots of reactions to lots of drugs which had to be discontinued. Your doctor relies on you to report everything untoward. Some of my common reactions: cramping in extremities, insomnia, weight gain, fatigue, nausea, etc.
Recently I was hospitalized for a serious viral respiratory infection. My treatment involved lots of steroids which are hard on your stomach. I fell the day I came home from the hospital and broke a rib, extending my recovery. I experienced gastrointestinal distress beyond my ability to cope, leading to a consultation with a gastroenterologist. He prescribed another pill. I didn’t have a lot of hope for this pill. In fact, five days into taking it, I wasn’t any better. But then I not only improved, I realized I was better than I had been for twenty years. I was amazed that a long-standing discomfort could be resolved, which put my head back on straight. I’ve been a much happier person since.
What We Wish Were True
 One of my dearest friends sent me a book for Christmas entitled, “What We Wish Were True”. I didn’t get to the book right away, but the title alone prompted much thought. The book is an autobiographical narrative about a young mother, Tallu Quinn, who has been diagnosed with a terminal brain cancer who struggles to reconcile her faith with her advancing disease and early death.
One of my dearest friends sent me a book for Christmas entitled, “What We Wish Were True”. I didn’t get to the book right away, but the title alone prompted much thought. The book is an autobiographical narrative about a young mother, Tallu Quinn, who has been diagnosed with a terminal brain cancer who struggles to reconcile her faith with her advancing disease and early death.
She articulates many of the same things I felt during the catastrophic phase of my illness 22 years ago. The loneliness and isolation of a critical illness, the awareness of a failing body, the abject sorrow of leaving those you love, the unfairness of an early death, and the suffering caused by caustic meds and painful procedures. Yet through it all, and within all, the author held an acute perception of love surrounding her, and beauty in the most ordinary things.
I wondered, what do we wish were true?
Perhaps most of all for folks who are victims of myocarditis, we wish we got to live in a world without pain, suffering, and loss: when we didn’t have to fight with insurance companies to cover the cost of our meds and procedures, or when we weren’t continually grieving an empty seat at our table.
We wish we were healthier. We wish that those who have passed were still with us. And we wish time would go backward to when life was simpler or happier. There is a big, bold black line between our pre-myocarditis lives and our post-myocarditis life, a moment in time when everything changed.
From a global perspective, we all wish there was a cure for myocarditis. We wish that cure had come in time to save our loved one or prevent us from suffering the pain of surgery or dealing with the uncertainty of waiting for an acceptable organ.
From a societal perspective, we might wish we weren’t having to cancel every event because a pandemic is looming and we are at risk of exposure due to immunosuppression, or we isolate because it seems we are the only ones who simply cannot not move on from our loss.
From a medical perspective, we wish drugs always worked, doctors were all compassionate, there were always enough nurses and beds available when we need to go to the hospital and that there were lots of drugs without deadly side-effects in the pipeline to help us.
But what is true?
That we have an appreciation for life, for ordinary things, for living in the moment, for the people we love, that we have an amazing capacity to embrace joy and that we live in a perpetual state of gratitude for our donor families.
That we have the comfort and fellowship of a family: a church family, a work family, a friend group, and at the very least, a medical team that stands behind us at every turn.
That there is a sincere generosity of spirit, compassion, kindness, and community when in the presence or conversation with other myocarditis victims. We speak honestly and openly to each other about our trials and tribulations and find comradery and support there.
While we try to cope with the reality of our lives and try to move on while not drawing too much attention to ourselves, the Myocarditis Foundation continues to work for a cure, funding research, keeping the public informed of new information on myocarditis, and supporting patients and families. While life continues to spin unpredictably around us, the Myocarditis Foundation is pressing on toward a brighter future.
Twenty Years
 A lot has happened in the almost 22 years since my heart transplant; some indelible, some forgettable. 2001, 911 happened while I was in the hospital in CCU pretransplant in Manhattan. 2003, the space shuttle Columbia made its first and last flight. 2005, Hurricane Katrina hit the southeast United States. In 2009, President Barrack Obama was inaugurated. 2012, Queen Elizabeth II celebrated her Diamond Jubilee. 2019, Tiger Woods claimed his fifth Masters title. In 2020, John Lennon’s Imagine was remastered and released. 2020 was heavily defined by the COVID pandemic, impacting every part of our lives.
A lot has happened in the almost 22 years since my heart transplant; some indelible, some forgettable. 2001, 911 happened while I was in the hospital in CCU pretransplant in Manhattan. 2003, the space shuttle Columbia made its first and last flight. 2005, Hurricane Katrina hit the southeast United States. In 2009, President Barrack Obama was inaugurated. 2012, Queen Elizabeth II celebrated her Diamond Jubilee. 2019, Tiger Woods claimed his fifth Masters title. In 2020, John Lennon’s Imagine was remastered and released. 2020 was heavily defined by the COVID pandemic, impacting every part of our lives.
In 2001, Dr. Les Cooper and I started working on the Myocarditis Foundation, officially receiving IRS approval in 2005. From my perspective, one of our greatest achievements has been in making “myocarditis” a household word. Now in 2023, in part due to COVID, not only the word but a rudimentary understanding of what it means permeates our culture. Dr. Cooper could articulate all the medical advances. In summary, we accomplished, with your help, almost everything we set out to do, except find a cure. So, our work continues.
In the past almost 22 years, some of my newer doctors look like they are the age of my children, yet I continue to be impressed with their skill in the practice of medicine. (This generation of doctors knows something about myocarditis.) Many of the doctors who have been with me from the beginning of my illness are now retired. Drug therapies haven’t changed much in 30 years. However, advances have been made in mechanical devices as well as in blood surveillance tools to monitor allograft health. New drug therapies without all the dreaded side effects, both long and short term, are on the horizon, but the approval process is very long.
Personally, these years have flown by; every year goes by even faster. For us transplants, the passage of time is both a blessing and a concern. Amy Silverstein passed away this week- 35 years out from two consecutive heart transplants, a few short weeks from the date her essay was published in the New York Times. If you go to her website, amysilverstein.com, she leaves a legacy of transplant advocacy which she describes as, “…an essential basis from which to address the longstanding unfavorable positioning and underfunding of research by NIH and FDA “. She suggests that you can impact research funding by sharing your #truthintransplant story with the largest organization of transplant professionals (American Society of Transplantation) by filling out the form on her website.
Maybe it is time for us to speak up.
The Gratitude Paradox
 As so many of you are well aware, I’ve recently been hospitalized with a respiratory virus. Those most at risk to serious outcomes of this virus are babies and immunosuppressed individuals. It’s been a very trying time for me and my family, coping with both the illness and the side effects of the medications used to treat the illness. This is not an unusual occurrence for heart transplant patients. We are always at risk for infections, rejections, vasculopathy and cancer due to the immunosuppression. Every hospitalization forces us to confront our very existence.
As so many of you are well aware, I’ve recently been hospitalized with a respiratory virus. Those most at risk to serious outcomes of this virus are babies and immunosuppressed individuals. It’s been a very trying time for me and my family, coping with both the illness and the side effects of the medications used to treat the illness. This is not an unusual occurrence for heart transplant patients. We are always at risk for infections, rejections, vasculopathy and cancer due to the immunosuppression. Every hospitalization forces us to confront our very existence.
On Tuesday, April 18, 2023, the New York Times published an Opinion/Guest Essay entitled, “My Transplanted Heart and I Will Soon Die”, written by Amy Silverstein, the author of Sick Girl. Amy has lived 35 years with two different donor hearts. She honored her hearts with “compulsive compliance” with the strictest interpretation of transplant protocols. Despite maintaining “sparkling cardiac health”, she is dying of metastatic lung cancer, a consequence of long-term immunosuppressive drugs. Her essay is a cry for better medications, greater life-expectancy from current protocols which she describes as antiquated and more attention to utilization of organs she feels are being wasted given current policies.
I’ll let you find and read the entire article if you wish. I would recommend it because she has a lot to say about the state of transplant medicine which impacts us all. She points out a pressure for transplant recipients to not express, much less demand medicines that allow for a longer, healthier life. She feels like this narrative discourages transplant recipients from talking freely about the compromising, life-threatening side effects of medicines we must take. She calls it “the gratitude paradox”.
My take on this is that besides our closest family and friends the “miracle” narrative prevents the public from really understanding how difficult being a transplant really is. It must be easy to live this way because we make it look that way. It isn’t. I am consistently unreliable in my attendance. I’m often in isolation at home for weeks at a time. And I don’t sleep well given the drugs. My family worries, my church supports me in prayer and my best friends thankfully text often.
Amy closes her article by sharing a conversation with her doctor, who sat in front of her crying upon sharing the diagnosis and prognosis of her cancer. With wry humor, Amy said, “I sacrificed my whole body for this heart. I kept her perfect to the end.” This forces me to say that it doesn’t seem fair.
It is anathema to my personality to see my transplant as anything other than a miracle. However, I can’t help but thank Amy for her last-ditch efforts to challenge the heart transplant system, to tell her truth, and for trying to make the transplant world better for those of us still fighting for every day and those to come; I wish her Godspeed.
Life-Saving Transplant Drugs: The Bane of Our Existence
Every Monday for the past 21 years, I’ve “poured” my medications for the week into my 7 daypill dispenser. The dispenser is a lifesaver because it helps me track whether I’ve taken my drugs or not. On any given day, depending on how healthy I am, I take a minimum of 17 pills in the morning and another 10 pills twelve hours later. I also have a cadre of “prn” meds to take “as needed” to help me through minor crises and a bunch of inhaled medications to treat an asthma exacerbation or respiratory issue. If you are new at this or the least bit confused about whether your symptom is minor or not, report it immediately to your doctor, and wait for instructions.
There are yellow warning labels on the side of the medication bottles that say, “May cause nausea (check), dizziness (check), diarrhea (check); or there may be other warnings, “Don’t eat grapefruit”, “ Don’t drive”, “May decrease effectiveness of birth control”, “Avoid pregnancy”, “Take with food or milk”, “Avoid contact with people with contagious diseases”, “Avoid exposure to sunlight”, “Check with doctor before drinking alcohol”, or “Do not skip doses”, to name a few. Take all those warnings seriously. Just for your own edification, ask your pharmacist for the pharmaceutical package insert, which lists whole host of other warnings, like “weight gain” (check), “insomnia (check) and even “psychosis” (sadly, check). If the side effects upset you, scare you, or leave you feeling insecure, call your transplant team. The most important point I want to make is that if you are having symptoms of any kind, that are NOT listed on the bottle or the insert, it doesn’t mean those symptoms are not happening to you-report them to your doctor anyway and stand firm in your reporting. Medical practitioners are constantly learning from our experiences.
Pharmacists will often change vendors and buy the cheapest generic form of the drugs. I am assuming they are more profitable. Many of the drugs we take are manufactured in third world countries that may or may not behave the same inside of you. I get tinnitus, ringing in the ears, from some generic brands of drugs by the same name. You’ll have a fight on your hands with your insurance company if you insist on taking the proprietary drug made in the US, because it costs more, but sometimes you must engage. Your transplant physician will help.
The biggest frustration with tracking the drugs is that the refills don’t come due on the same day necessitating frequent trips to your pharmacy. Lots of my drugs are on automatic refill but sometimes that doesn’t always work. Make friends with your pharmacist. Let them know when your refills are urgently needed, meaning you are completely out or let them know if you have a little leeway. Most drugs they can get by the next day, so plan ahead. We as transplants can’t afford to not take these drugs as directed. Our lives depend on it.
Candace Moose, Co-Founder of the Myocarditis Foundation
New Year, New You
 They say it’s important to have goals. My primary goal these past 21 years has been survival, and secondarily to leave the world a better place for future generations. The clock starts again in the New Year for all maintenance protocols that quantify my health and verify that all is as good as it can be. So, scheduling begins: Dermatology appointments to rule out skin cancer, quarterly visits with my Transplant Cardiologists, Dexa Scan to rule out osteoporosis and follow up visit with Endocrinology, Mammogram to rule out breast cancer, Opthalmology to check for glaucoma and cataracts which are common side effects of transplant drugs, Interventional Cardiology visit to check defibrillator device, every five years with Gastroenterology to schedule a colonoscopy, to name a few.
They say it’s important to have goals. My primary goal these past 21 years has been survival, and secondarily to leave the world a better place for future generations. The clock starts again in the New Year for all maintenance protocols that quantify my health and verify that all is as good as it can be. So, scheduling begins: Dermatology appointments to rule out skin cancer, quarterly visits with my Transplant Cardiologists, Dexa Scan to rule out osteoporosis and follow up visit with Endocrinology, Mammogram to rule out breast cancer, Opthalmology to check for glaucoma and cataracts which are common side effects of transplant drugs, Interventional Cardiology visit to check defibrillator device, every five years with Gastroenterology to schedule a colonoscopy, to name a few.
The New Year is also a great time to re-evaluate and reset your diet and fitness goals. Depending on bloodwork and cath results, which determine whether your commitment to fitness and diet is required or imperative. I find it very hard for me to keep a fitness routine, as overuse of a repetitive exercise often leads to injury and a stint with Physical Therapy. It’s also very hard for me to keep a stable weight, given medication, balance issues, susceptibility to infections, and issues that side-line an exercise program, my best intentions to move are easily compromised. The overall goal, however, is to just keep trying, adjusting, and adapting. According to the wisdom of Winston Churchill, “Never, never, never give up.”
Then there are New Year quality of life type goals: travel, hobbies, special celebrations, new jobs. I am the eternal optimist. I keep making travel plans that ultimately get cancelled because of the virus or injury or transplant issue du jour. But again, don’t give up. Keep trying.
My sister recently passed following a long battle with breast cancer. In those 36 years, she made every minute of her life count. She climbed mountains, hiked, camped, and kayaked as often as she could. I’m a hotel person, myself, not a camper. The moral of the story? Make it count. Do everything you can to become or get healthy. It’s a gift that requires work.
Holidays 2022
 This holiday season I wish you peace, peace in your body, your mind, and your spirit. There have been times in my transplant life when things were not peaceful. Sometimes it’s due to medications; medications that don’t let you sleep, make you irritable, or make you hungry. Some holiday seasons are filled with worry; having had tests and awaiting results, getting test results that indicate one of your other organs is not peaceful or perhaps you feel unsettled about an as yet unidentified health issue.
This holiday season I wish you peace, peace in your body, your mind, and your spirit. There have been times in my transplant life when things were not peaceful. Sometimes it’s due to medications; medications that don’t let you sleep, make you irritable, or make you hungry. Some holiday seasons are filled with worry; having had tests and awaiting results, getting test results that indicate one of your other organs is not peaceful or perhaps you feel unsettled about an as yet unidentified health issue.
Sometimes holidays are difficult because of life stressors that have nothing to do with being a transplant; loss of loved ones, financial instability, or relationships gone awry. Not all holidays are merry and bright. If they are not, and you need help, reach out; there are always staff, professionals, hot-lines, and emergency personnel available to help. Share with someone that your need help.
However, if you are good, reach out to others with a message of Holiday cheer. Make someone else merry. Help others; donate to Food Banks, volunteer, or walk dogs at an animal shelter. Nothing helps me forget about my own issues like doing something for others. Foster peace in your spirit and in your life. I believe it contributes to good health. Peace is a valuable commodity, perhaps the most valuable. So Happy Peaceful New Year!
Candace Moose
Co-Founder The Myocarditis Foundation
The Challenges of the Holidays
November 28, 2022
 There is no question, the holidays are my favorite time of year. I love the lights, the decorations, the gift giving and receiving, the hustle and bustle, all the holiday-themed movies and of course the spirit of love that pervades the very air we breathe. However, the holidays present many challenges to victims of myocarditis. But try as we might, all holidays don’t work out as planned. For those who have experienced loss, there is always an empty seat at the table.
There is no question, the holidays are my favorite time of year. I love the lights, the decorations, the gift giving and receiving, the hustle and bustle, all the holiday-themed movies and of course the spirit of love that pervades the very air we breathe. However, the holidays present many challenges to victims of myocarditis. But try as we might, all holidays don’t work out as planned. For those who have experienced loss, there is always an empty seat at the table.
My first holiday after the heart transplant, to be honest, was a sad affair. I think we were all suffering from PTSD that would take years to resolve. I went home from the hospital on IV chemotherapy which had to be discontinued in early December because my white cell count was too low, which meant no family gatherings. We are a loud and ruckus group, my family, with a penchant for fun and overindulgence, so to add insult to injury, after all we had been through, a quiet affair with just my husband, son, and I, seemed unfair. Yet, I was alive, while others had not survived. Even today, as I hang ornaments on my tree, I think of the parents of Brad, Rhett, Andy, Danielle, Sarah, Michael, and far too many others, and it breaks my heart. Thinking of them motivates me give more of my time and resources to the Foundation.
17 years later, I was hospitalized in isolation during the holidays in New York, with an esoteric, contagious respiratory virus. When I looked out the window of my hospital room on Christmas day, not one car was parked either side of the street. It was apocalyptic. But it did snow, and that small thing lifted my heart. My husband was situated in a family hospital housing room upstairs. He too became desperately ill as the week progressed, diagnosed in the ER with a respiratory virus; not the same one I had, so we couldn’t see each. It was a comfort just knowing he was there. Our children and grandchildren missed us terribly, and we them. I remember turning on my TV to watch the burning log and listen to Christmas carols. I remember feeling so grateful that I had a family who loved me, even if from afar. The Holidays, a season of love, near or far, on earth and in heaven.
The emotional and physical toll a catastrophic disease like Myocarditis takes on both the patient and their families are immeasurable. The physical insult takes time to resolve but the emotional toll, especially for those who have experienced loss, is immeasurable. The Myocarditis Foundation is here for you. We have been working for many years to educate the public about this once considered rare disease. Help us collect data for publication by participating in our Emotional Toll study, conducted in partnership with the Mayo Clinic. Participation information can be found on our website: myocarditisfoundation.org or by calling our Executive Director Gen Rumore. Happy Holidays, dear ones.
My Good Life
October 25, 2022
 Next month I’m headed to Mayo Clinic in Jacksonville, Florida, to visit my old heart, which resides in the office of my Myocarditis Foundation Co-Founder, Dr. Leslie Cooper. I donated my old heart to his research when I was well enough to understand the contribution his research meant to my recovery. I remember asking Dr. Deng when I woke up after the transplant surgery if it really needed to be replaced. Somehow, after all I’d been through, I had trouble believing it had failed me.
Next month I’m headed to Mayo Clinic in Jacksonville, Florida, to visit my old heart, which resides in the office of my Myocarditis Foundation Co-Founder, Dr. Leslie Cooper. I donated my old heart to his research when I was well enough to understand the contribution his research meant to my recovery. I remember asking Dr. Deng when I woke up after the transplant surgery if it really needed to be replaced. Somehow, after all I’d been through, I had trouble believing it had failed me.
For fifty years, I had depended on that heart, and it had never let me down. My father always said I wore my feelings on my sleeve, but the truth was, my heart took the lead in all decisions made in my life up to that point. My heart had served me well. It chose wisely my husband of 50 years. It guided me in my career choice of becoming a nursing. I chose a host of wonderful friends with my heart, and they chose me back because of my heart. Several people said to me after the transplant, “I can’t believe they had to replace your heart, because your first one was so beautiful!”.
Mine is the kind of heart that cries for joy: when an Olympian wins a medal, when a marathoner finishes a race, when an actor wins an Academy Award, when someone performs an unexpected, random act of kindness. Mine is the kind of heart that cries when people get married, or a baby is baptized. My heart believes that good always wins in the end.
I’m a believer in the power of love to save, to heal, to restore, and to forgive. The heart is the organ of love, in poetry, music and art. Yet in all those years, I’d never seen my damaged heart. And now is the time. I have a lot to thank it for. I expect the experience to be an emotional one, but a healing one.
The Aging Heart
September 26, 2022
 October 1st is the 21st anniversary of my heart transplant. We call it our rebirthday, the day we were given a second chance to live. What a wild and wonderful ride it has been. I’ve done everything I could do over these past years to keep this heart healthy medically, physically, and spiritually, and I’ve been given so much. But the heart is aging anyway.
October 1st is the 21st anniversary of my heart transplant. We call it our rebirthday, the day we were given a second chance to live. What a wild and wonderful ride it has been. I’ve done everything I could do over these past years to keep this heart healthy medically, physically, and spiritually, and I’ve been given so much. But the heart is aging anyway.
It’s curious to find myself at this point in life even though I knew all along that it was coming, that there was an endpoint. How do we deal with it? I suggest no differently than we’ve handled our transplanted life: with positivity, with courage, and with an understanding that we never were in control anyway. We stumble, we fall, we get discouraged, we struggle to hold up under treatments and procedures that make us crazy, cause us pain, or make us sick. Sometimes, the worst parts are temporary. Ask for help, be that for medication, support, or prayers from medical professionals, friends, and churches. Count on those you can count on in your life.
No one can really understand this transplant life except those of us who live it. But you are not alone. Your transplant team stands ready to stand with you. Don’t hesitate to reach out, in fact, fight to be heard if you must, but speak up.
Transplant is not the best answer to treat myocarditis. It was the only treatment available to us at the time. It was never intended to be a cure. It remains a temporary solution. More diagnostics leading to early diagnosis and more treatments administered earlier in the disease process before the heart is damaged beyond recovery, is the answer. Give generously to The Myocarditis Foundation. Help us fund more research.
21 Years as an Advanced Heart Failure Patient
August 29, 2022

It’s hard to write when you in the middle of a crisis, but that is where we live as heart transplants: crisis to crisis. Life, wonderful life, seems to clip along for a period of time, and then, all of a sudden it doesn’t. No matter the issue at hand, we do our best to understand it medically and to cope with it psychologically.
I am celebrating 21 years post-heart transplant on October 1st. When folks ask how I am doing, to most casual acquaintances, I answer vaguely that I am currently experiencing some issues. Lots of my contemporaries are experiencing all kinds of serious health issues for the first time in their lives; so, it is not unusual to hear friends describe a health issue at my age in response to the question, “How are you doing?”. I’ve been labeled an Advanced Heart Failure patient for 21 years and have required frequent medical attention. A common response is, “Well, you’ve certainly have had a good run.” True indeed.
I’ve seen my children married to wonderful spouses and enjoyed being part of my grandchildren’s lives. I’ve tried to make a difference by co-founding The Myocarditis Foundation with Dr. Leslie Cooper. And I’m very grateful to Gen and Joe Rumore for taking over the leadership of the foundation when I stepped back from day-to-day operations. Their commitment is palpable. We’ve helped many people, advanced the science by awarding research grants, and contributed to making “myocarditis” a household word, thanks in part to COVID. My particular life-long passion has been mission work. I am a heart transplant because of the two immunizations I was required by the CDC to have before leaving on a mission trip to Africa-a trip that never happened because of 9/11 and because I became catastrophically ill with an autoimmune form of myocarditis. I’ve enjoyed public speaking on topics that are important to me: organ donation, The Myocarditis Foundation, my faith, and mission projects.
I’ve met a lot of very special people along the way: doctors, nurses, other heart transplant patients, parents who have lost children to myocarditis, siblings who have lost siblings, friends who have lost friends. We understand, as much as possible, each other’s suffering. Lines between doctors and patients are blurred. We have access to information and support, from medical professionals and each other. People said I had a good heart to begin with. My new heart is even better.
It’s been fascinating watching the field advance over the years, meeting executives and founders of companies that are developing treatments and diagnostic tools to support myocarditis patients. There is still much to do to eradicate this disease, but progress is being made.
Yes, I’ve have had a very good run, but I’m not done yet. In fact, I’m going for a record. As Tom Petty so famously sang in his song “Swingin’”, “I’m goin’ down swinging, like Sonny Liston.”
Candace Moose
Heart Transplant: Owner’s Manual
July 28.2022
 I think the human body is far more complicated than people realize, especially when diagnosed with myocarditis and Giant Cell Myocarditis. We’re all as different on the inside as we are on the outside. I remember Dr. Deng saying we’re not like cars. When you lift the hood, we are not the same. As well, our journeys are very similar yet very different. Transplant anti-rejection medication cocktails must be customized to each individual patient. I never met another heart transplant who was on the same medication regime as me. Nor have I ever met another patient who has rejected as much as I have. (Rejection is the presence of white blood cells in the tissue sample that is removed from the inside of the heart during a biopsy. The presence of WBCs in the tissue means that the body is recognizing the heart as foreign which is treated with increased medication). Likewise, I probably have had more biopsies than others because of all the rejections; and downstream, more steroids. Thanks to the development of Allomap, a simple blood test for rejection which became standard of care in 2010, many of us have far fewer biopsies. All this doesn’t make me special, but it does make me complicated. There are a myriad of reasons why you are incredibly complicated as well and require special treatment.
I think the human body is far more complicated than people realize, especially when diagnosed with myocarditis and Giant Cell Myocarditis. We’re all as different on the inside as we are on the outside. I remember Dr. Deng saying we’re not like cars. When you lift the hood, we are not the same. As well, our journeys are very similar yet very different. Transplant anti-rejection medication cocktails must be customized to each individual patient. I never met another heart transplant who was on the same medication regime as me. Nor have I ever met another patient who has rejected as much as I have. (Rejection is the presence of white blood cells in the tissue sample that is removed from the inside of the heart during a biopsy. The presence of WBCs in the tissue means that the body is recognizing the heart as foreign which is treated with increased medication). Likewise, I probably have had more biopsies than others because of all the rejections; and downstream, more steroids. Thanks to the development of Allomap, a simple blood test for rejection which became standard of care in 2010, many of us have far fewer biopsies. All this doesn’t make me special, but it does make me complicated. There are a myriad of reasons why you are incredibly complicated as well and require special treatment.
Our Advanced Heart Transplant Team is challenged to practice their craft on our ever-changing presentation over time, as well, meaning, the challenges we face in year one are very different than the challenges patients face a decade or two out. And believe me, I don’t pretend to understand it all. I do my best to keep up: I ask lots of questions, keep my doctor informed about what’s different and ultimately leave my care up to my doctor to figure out.
At twenty years, my care is all about maintenance while keeping an eye on the effect of years of harsh drugs on my vital organs and ruling out cancers which are more prevalent when immunosuppressed. Sometimes it’s hard to keep up with these old bones: Dermatology twice a year to rule out skin cancer (I’ve had 5 Moh’s procedures), Bones Densities to track effect of calcium leaching steroids, Dentist twice a year to keep gums healthy, Colonoscopies, Mammographies, to name a few, and follow-up on persistent medical issues that were present prior to being a transplant. Yikes!
Sound impossible? You bet, but because it’s so important, you will do it. For yourself; for your donor; for every family that has a loved one who didn’t make it but are rooting for your success.
Read Candace’s Story of her Transplant Games
June 22, 2022
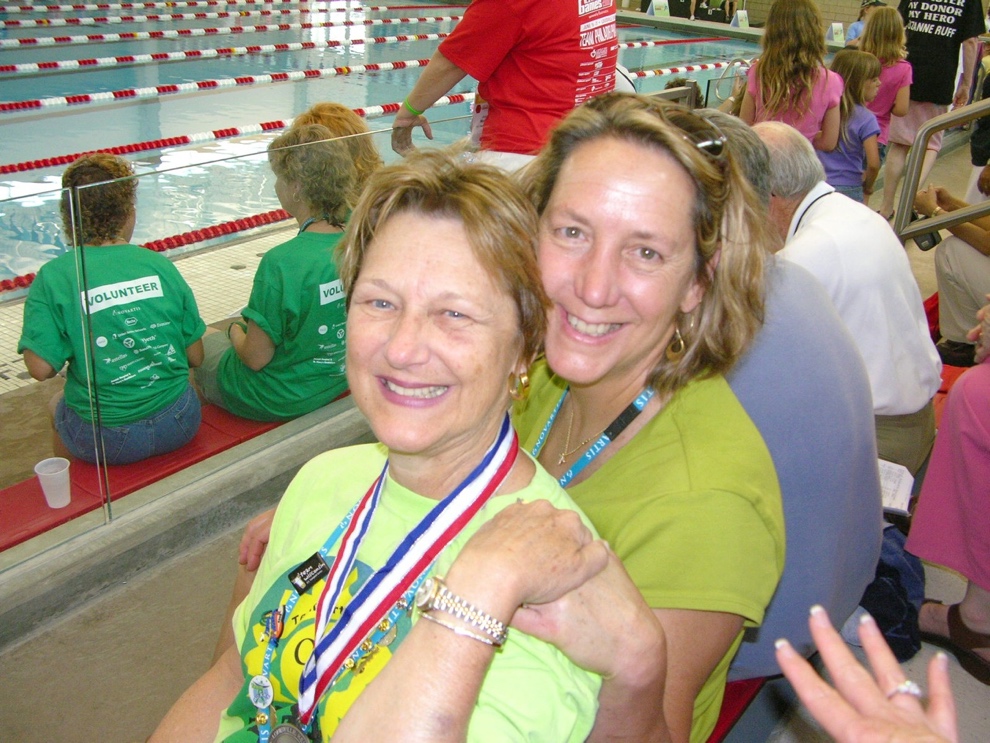 While living in Raleigh, I had the opportunity to participate in the National Transplant Olympics in Louisville, Kentucky, as a member of team North Carolina. The team was sponsored by the state chapter of the National Kidney Foundation. The team had to raise the money for all 30 of us (with chaperones for children) to go for three days: airfare, hotels, meals, and uniforms (tee shirts). I co-chaired a poker night at Brier Creek Country Club, with the help of many friends, neighbors, and Team NC teammates, and raised $30,000., enough to cover all our expenses for the next Olympics two years later in Pittsburg. It was an exhilarating evening.
While living in Raleigh, I had the opportunity to participate in the National Transplant Olympics in Louisville, Kentucky, as a member of team North Carolina. The team was sponsored by the state chapter of the National Kidney Foundation. The team had to raise the money for all 30 of us (with chaperones for children) to go for three days: airfare, hotels, meals, and uniforms (tee shirts). I co-chaired a poker night at Brier Creek Country Club, with the help of many friends, neighbors, and Team NC teammates, and raised $30,000., enough to cover all our expenses for the next Olympics two years later in Pittsburg. It was an exhilarating evening.
All the participants in the Olympic competition were solid organ transplants: heart, lungs, liver, kidney, intestines, and pancreas. Some of the participants were children, some blind, some amputees, surgical scars visible on most everyone. Emotional scars not as obvious. All of us on immunosuppressive drugs, feeling lucky, fragile, and grateful. The kickoff event is the Parade of Athletes by state in uniform preceded by the donor families under their own banner, the people who made it possible for us to live, welcomed by a standing ovation and an avalanche of tears.
Team North Carolina was coached by a wonderful man Bill, a kidney transplant himself; a great man and a dear friend. I didn’t know exactly where I would fit in; I just knew I needed to be there. I was thinking egg toss, only to discover this was not an event. Coach Bill found a place for me in two relay swim events doing the backstroke. The other three women on the team were all experienced and very talented competitive swimmers; some even swam on college teams. I grew up swimming in my grandmother’s backyard pool. Of course, I could do a backstroke! What I couldn’t do was the underwater flip turn. In turning, I lost my sense of direction and couldn’t tell which way was up. I was afraid I would drown, what Simone Biles, gymnast, described as the “zoomies” when she feared losing her sense of direction, so she declined to participate in some of the 2022 Chinese Olympics. The referees made a special accommodation, allowing me to turn at the wall, my head above water. Special accommodations were made for every competitor who needed one, because the point was to participate, to finish, but not to win. Despite my personal unimpressive results, because my teammates were so skilled, I won two silver medals. My late sister, Mary Ann, my ever-present cheerleader, since then a victim of breast cancer, was there to support me. I couldn’t have done it without her.
Well, Team NC won the national competition that year; we took first place!! Many of us didn’t even realize it was a national competition, much less being aware that we were winning so many events. That is what made it so wonderful.
Heart Disease in Women
May 12, 2022
 I think all my physicians would agree that my Giant Cell Myocarditis was the result of my body’s reaction to two immunizations. The early published medical literature though sparse documented some cases of GCM due to immunizations. The simplest way to explain it is that there were some cells on the surface of my heart that were very similar to the immune cells the immunization antigen was supposed to bond with, causing my body to try to destroy my heart. All my life, I had weird reactions and over-reactions to drugs, so I took very few of them and only when necessary. I had retired from 29 years in a variety of nursing positions and was looking forward to doing short term missionary work in Africa.
I think all my physicians would agree that my Giant Cell Myocarditis was the result of my body’s reaction to two immunizations. The early published medical literature though sparse documented some cases of GCM due to immunizations. The simplest way to explain it is that there were some cells on the surface of my heart that were very similar to the immune cells the immunization antigen was supposed to bond with, causing my body to try to destroy my heart. All my life, I had weird reactions and over-reactions to drugs, so I took very few of them and only when necessary. I had retired from 29 years in a variety of nursing positions and was looking forward to doing short term missionary work in Africa.
Almost one year exactly from the date of my retirement, I had two immunizations required by the CDC to travel to that part of the world to prevent me from acquiring diseases that we do not have in the U.S. Two hours after the immunizations, my heart began to misbehave, beating too rapidly, too irregularly and too forcefully. I was a healthy 49-year-old who logged at least 10 miles per week with vigorous walking for years and that summer had spent evenings crewing on Long Island Sound. We have no vascular heart disease in the family. So, I didn’t expect a heart issue; I thought it was menopause. It was a Friday, there was no cause for alarm, so I went about my life. As the days progressed, my heart symptoms were less subtle and persistent then advanced to shortness of breath on exercise.
Early in my nursing career I had worked in CCU. Almost all of patients were male and had experienced crushing chest pain, radiating down an arm and profuse sweating. I had none of that. My husband made me go to our Family Doctor when I came back from my walk and was short of breath. He offered to take me; I said confidently “no”, I was fine and could handle it myself.
I was at the doctor when he opened at 9 am. My EKG result was grossly abnormal so I was admitted to the ER, and subsequently a cardiac floor until EMT transport could be arranged to transfer me to the closest interventional heart hospital for supposed bypass surgery. I was finally convinced this was a real problem when the first set of bloodwork done in the ER revealed an extremely high Troponin-an enzyme that is released into the bloodstream when the heart muscle is damaged. It was all downhill from there, a story likely very similar to every other myocarditis patient who ended up being transplanted.
I wrote this story today to emphasize that women experience heart disease differently than men and therefore delay in seeking treatment. Heart disease is the #1 killer of women in the U.S., with even more alarming statistics for African American women, perhaps related to a cumulative lack of access to healthcare throughout their lives. Because our symptoms are generally more subtle, GI upset, pain in jaw, fatigue, to name a few, and because we’re so busy putting other people’s needs ahead of our own, statistics prove that women do not seek care as quickly as they should. Yes, myocarditis or inflammatory heart disease is decidedly different than vascular heart disease, but I postulate that some of the same behaviors of not seeking care as soon as they should, applies here as well. My delay could have cost me my life, and almost did.
For additional resources, please go to the American Heart Association website and search for the Go Red for Women campaign to learn more. * The Myocarditis Foundation has co-funded several grants to study myocarditis with AHA.
The Gift of a Good Doctor
April 12, 2022

Giant Cell Myocarditis Survivor Dedicated Her Life to Saving Others
Candace Partnered with Two Doctors to Form the Myocarditis Foundation
 In August 2001 I received two immunizations to travel to Africa to do mission work. Two hours later, my heart started to beat faster, more irregularly and more forcefully. One week later I coded three times, had a defibrillator inserted and was sent home with a diagnosis of viral myocarditis.
In August 2001 I received two immunizations to travel to Africa to do mission work. Two hours later, my heart started to beat faster, more irregularly and more forcefully. One week later I coded three times, had a defibrillator inserted and was sent home with a diagnosis of viral myocarditis.
The next day I went into cardiogenic shock and though the doctors told my husband there was only a slim chance I would survive the night, if by some miracle I did, my only chance for survival was a heart transplant.
The next day, I was transported via EMT to Columbia Medical Center where Dr. Deng was waiting for me in the Critical Coronary Unit.
He knew immediately it was giant cell myocarditis and he consulted with the world’s leading expert, Dr. Leslie Cooper from the Mayo Clinic.
Dr. Cooper’s research showed that by giving chemotherapy because of its immunosuppressant and anti-inflammatory properties, GCM patients survive until transplant if a heart were to become available. In all those weeks, I laid in my bed in the CCU praying that I would live to see my children married and my grandchildren born.
The treatment was successful and a heart did come on October 1, 2001; the heart of a 17 year old boy whose parents made an unbelievably difficult decision to donate their son’s organs. I survived only because of a series of miracles: Dr. Deng’s immediate diagnosis of Giant Cell, Dr. Cooper’s research and treatment recommendations and the gift of a heart from an unknown family who suffered tremendous loss.
I said to Dr. Deng and Dr. Cooper, “What can I do to give back to you what your knowledge, expertise and care have given to me?” Together, we formed the Myocarditis Foundation to help other patients and families in the present. It is our hope that the research we fund will result in more lives saved in the future. I plan to work toward that goal for the rest of the life I am given.